NJ (908) 688-5577
NY (212) 737-2528
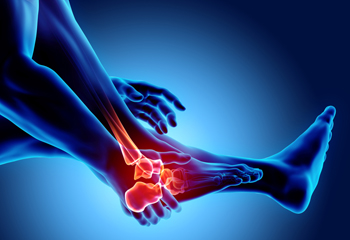
Foot arthritis, a multifaceted condition, manifests in various ways, each presenting distinct challenges for those grappling with joint inflammation in the feet. Osteoarthritis, the most common form, results from wear and tear on the joints, causing pain and stiffness. Rheumatoid arthritis, an autoimmune disorder, targets the joints and may lead to deformities in the feet. Gout, characterized by the accumulation of uric acid crystals, induces sudden and severe pain. Recognizing the specific type of foot arthritis is essential for implementing targeted relief methods. While medications are common approaches to treatment, lifestyle modifications such as maintaining a healthy weight and choosing supportive footwear can help to alleviate symptoms. Resting the feet and engaging in gentle exercises can provide relief. Foot arthritis can cause discomfort, and if you are suffering from this condition, it is suggested that you visit a podiatrist who can guide you toward effective relief methods.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact the doctors from Advanced Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a term that is commonly used to describe joint pain. The condition itself can occur to anyone of any age, race, or gender, and there are over 100 types of it. Nevertheless, arthritis is more commonly found in women compared to men, and it is also more prevalent in those who are overweight. The causes of arthritis vary depending on which type of arthritis you have. Osteoarthritis for example, is often caused by injury, while rheumatoid arthritis is caused by a misdirected immune system.
Symptoms
Arthritic symptoms range in severity, and they may come and go. Some symptoms stay the same for several years but could potentially get worse with time. Severe cases of arthritis can prevent its sufferers from performing daily activities and make walking difficult.
Risk Factors
If you suspect your arthritis is affecting your feet, it is crucial that you see a podiatrist immediately. Your doctor will be able to address your specific case and help you decide which treatment method is best for you.
If you have any questions please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
During your lifetime, you will probably walk about 75,000 miles, which is quite a lot of stress to put on your feet. As you get older, the 26 bones and 30 joints in each of your feet will lose flexibility and elasticity. Your foot’s natural shock absorbers will wear down as well. Having arthritis added to this mix only makes matters worse. Your joints will become distorted and inflamed, which is why arthritic foot care needs to be something to think about every day.
When dealing with arthritis, having additional foot complications, such as bunions, hammertoes, or neuroma, can be a serious detriment. To avoid these, buy well-fitting shoes with a lower heel and good support. Arthritis causes you to lose your arch, so having shoes with good arch support is also highly recommended.
Aside from getting good arch support, the shoes need to fit comfortably and properly as well. A good place to start is by leaving a finger width between the back of the shoe and your foot to gauge proper size. It is also helpful to have a square or rounded toe box in the front to provide even more comfort. Another thing to look for is a rubber sole that can provide a cushion and absorb shock as you walk. This adds flexibility to the ball of your foot when you push off your heel to walk.
Exercise is another key aspect of arthritic foot care. Exercise not only strengthens and stretches your muscles and joints, but helps to prevent further injury and pain as well. Stretching the Achilles tendon, the tendon located in the back of your heel, will give you added mobility and reduce pain due to stress. Another thing you can do is massage your feet, kneading the ball of your foot as well as your toes from top to bottom.
Stretching the Achilles tendon is a simple exercise that you can do at home anytime. Lean against the wall with your palms flat against the surface while placing one foot forward, towards the wall, and one foot behind you. Bend your forward knee towards the wall while keeping your back knee locked straight, and make sure both your heels are completely touching the ground at all times. This will stretch your Achilles tendon and calf muscles as well. You will feel the stretch almost immediately. You can also stretch your toes in a couple ways. One involves taking a rubber band and wrapping it around both your big toes while your heels remain together. Then, pull them apart to stretch your big toe. You can also place a rubber band around all the toes of one of your feet. Then, try to separate each individual toe, stretching them all.
A final step you can take to help your arthritis is taking non-steroid, non-inflammatory drugs or topical medicines with capsaicin. Unfortunately, there is no complete way to remove all of your arthritic pain. However, following some of this advice can go a long way in staying as pain-free as possible.
Athlete's foot, a common fungal infection that affects the skin of the feet, can be influenced by various environmental factors. Moisture plays a significant role in its development, as the fungus thrives in warm, damp conditions. Sweaty feet trapped in tight, poorly ventilated shoes or damp environments, like locker rooms and communal showers, create an ideal breeding ground for the fungus. Therefore, keeping your feet dry and clean is essential in preventing athlete's foot. Furthermore, sharing contaminated surfaces, such as towels or footwear, can contribute to its spread. It is critical to practice good foot hygiene and avoid sharing personal items with infected individuals to reduce the risk. Preventive measures include wearing breathable shoes, changing socks regularly, and using antifungal powders or creams. Proper foot hygiene and avoiding exposure to fungus-prone areas are key in reducing the likelihood of athlete's foot. If you have developed athlete’s foot, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with the doctors from Advanced Podiatry. Our doctors will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Athlete’s foot is a type of fungal infection that affects the skin on the feet. It is caused when the tinea fungus grows on the foot. It is possible to catch the fungus through direct contact with someone who has it or by touching a surface that is contaminated with it. This type of fungus thrives in warm, moist environments such as showers, locker room floors, and swimming pools. Your risk of getting it may also increase by wearing tight-fitting, closed-toe shoes, or by having sweaty feet.
Symptoms of athlete’s foot include itching, stinging or burning sensations between the toes. You may also experience toenails that are discolored, thick, crumbly, or toenails that pull away from the nail bed.
Your podiatrist may diagnose athlete’s foot by detecting these symptoms or by doing a skin test to see if there is a fungal infection present. The most common exam used to detect Athlete’s foot is a skin lesion potassium hydroxide exam. To use this method, your doctor will scrape off a small area of the infected skin and place it into potassium hydroxide. The potassium hydroxide will destroy the normal cells and leave the fungal cells untouched so that they are visible under a microscope.
There are a variety of treatment options for athlete’s foot. Some medications are miconazole (Desenex), terbinafine (Lamisil AT), clotrimazole (Lotrimin AF), butenafine (Lotrimin Ultra), and tolnaftate (Tinactin). While these options may be able to treat your fungus, it is best that you consult with a podiatrist in order to see which treatment option may work best for you.
In some cases, Athlete’s foot may lead to complications. A severe complication would be a secondary bacterial infection which may cause your foot to become swollen, painful, and hot.
There are ways that you can prevent athlete’s foot. Washing your feet with soap and water each day and drying them thoroughly is an effective way to prevent infections. You also shouldn’t share socks, shoes, or towels with other people. It is crucial that you wear shower sandals in public showers, around swimming pools, and in other public places. Additionally, you should make sure you wear shoes that can breathe and change your socks when your feet become sweaty. If you suspect that you have Athlete’s foot, you should seek help from a podiatrist as soon as possible.
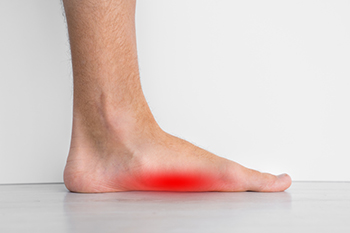
Living with flat feet, a condition characterized by the absence of arches on the feet, can be a lifelong experience starting in childhood. When someone with flat feet stands, their entire foot touches the ground, though in most cases, it does not lead to harm. However, some individuals may experience symptoms such as swollen ankles, difficulty standing on their toes, or pain in the foot arch area. Identifying these signs, particularly in children, is important for early intervention. While flat feet can be a natural part of a child's development, it can also develop later in life from age related factors. Seeking medical attention involves a comprehensive examination, where a podiatrist may recommend custom shoe inserts and certain exercises to alleviate discomfort. In severe cases, surgery may be considered. Home care includes minimizing stress on the feet, weight management, and, if necessary, pain relief measures. If you are experiencing discomfort related to flat feet, it is suggested that you schedule an appointment with a podiatrist for a full exam and suggested treatment measures.
Flatfoot is a condition many people suffer from. If you have flat feet, contact the doctors from Advanced Podiatry. Our doctors will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Flatfoot is a foot disorder that is not as straightforward as many people believe. Various types of flatfoot exist, each with their own varying deformities and symptoms. The partial or total collapse of the arch, however, is a characteristic common to all types of flatfoot. Other signs of flatfoot include:
One of the most common types of flatfoot is flexible flatfoot. This variation usually starts in childhood and progresses as one ages into adulthood. Flexible flatfoot presents as a foot that is flat when standing, or weight-bearing. When not standing, the arch returns. Symptoms of flexible flatfoot include:
Your podiatrist will most likely diagnose flatfoot by examining your feet when you stand and sit. X-rays may be taken to define the severity and help determine the treatment option best for your condition. Nonsurgical treatments can include activity modification, weight loss, orthotics, immobilization, medications, physical therapy, shoe modifications, and ankle foot orthoses (AFO) devices. If nonsurgical methods prove ineffective, surgery may be considered. Multiple surgical procedures can correct flatfoot; and depending on your specific condition, one may be selected alone or combined with other techniques to ensure optimal results.
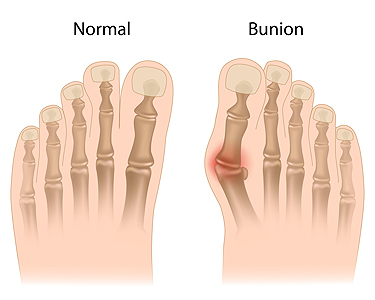
A bunion, a prevalent foot deformity, draws attention to the joint at the base of the big toe, where a bony bump forms. This condition, known as hallux valgus, gradually develops when the big toe leans inward toward the second toe, causing the metatarsal bone to protrude. Bunions can result from genetic predisposition, wearing ill-fitting shoes that squeeze the toes, or conditions such as arthritis. The gradual misalignment of the toe joint leads to inflammation, pain, and, in some cases, difficulty in finding comfortable footwear. While bunions are often associated with discomfort and aesthetic concerns, they can also impact joint function over time. Understanding the overview of bunions involves recognizing the factors contributing to their development and the potential implications on foot health. If you have a bunion, it is suggested that you visit a podiatrist who can guide you toward effective relief options.
If you are suffering from bunion pain, contact the doctors of Advanced Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
Symptoms
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.

An ankle sprain occurs when ligaments are damaged due to a sudden incident, often when the foot rolls or twists beyond its usual range. This can result in the overstretching or tearing of ligaments. An inversion sprain causes strain on the outer ligaments and an eversion sprain affects the inner ligaments. Treatment for the majority of uncomplicated ankle sprains involves rest, avoiding weight on the ankle for the first 48 hours, compression using an elastic bandage, and elevating the foot to reduce swelling. If the ankle swells severely right after the injury and bearing weight is impossible, it is suggested that you schedule an immediate appointment with a podiatrist. Other signs for urgent attention include a loud crack or pop during the incident or an ankle deformity unrelated to swelling. Complete rehabilitation of the ankle joint is essential to avoid developing chronic weakness that can lead to further sprains. Among measures that can help are performing a range of motion, balance, and strengthening exercises with guidance from a podiatrist on length of time and intensity. To ensure a tailored treatment plan for a sprained ankle, it is suggested that you make an appointment with a podiatrist.
Although ankle sprains are common, they aren’t always minor injuries. If you need your ankle injury looked at, contact the doctors from Advanced Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains are the result of a tear in the ligaments within the ankle. These injuries may happen when you make a rapid shifting movement while your foot is planted. A less common way to sprain your ankle is when your ankle rolls inward while your foot turns outward.
What Are the Symptoms?
Preventing a Sprain
Treatment of a Sprain
In many cases, the RICE method (Rest, Ice, Compression, and Elevate) is used to treat ankle sprains. However, you should see a podiatrist to see which treatment option would work best with your injury. In severe cases, surgery may be required.
It is important to ask your doctor about rehab options after you receive treatment for your injury. Stretching, strength training, and balance exercises may help the ankle heal while also preventing further injury.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.