NJ (908) 688-5577
NY (212) 737-2528
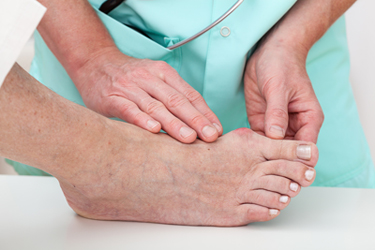 A bunion is a bony bump located on the outside of the big toe. The bump may be swollen, red, and irritated due to friction as it rubs against your shoes. Bunions deform the feet, making the first metatarsal foot bone stick out and causing the big toe to point towards the other toes. Thick, hardened skin or calluses often form on the second toe and underneath the big toe. A bunion can also make it difficult to find comfortable shoes, as they change the structure of the feet. They can also cause pain and discomfort while walking or standing. Bunions tend to get worse without treatment, so if you have bunions, it is suggested that you seek the care of a podiatrist to stop or slow their progression and get the right treatment for you.
A bunion is a bony bump located on the outside of the big toe. The bump may be swollen, red, and irritated due to friction as it rubs against your shoes. Bunions deform the feet, making the first metatarsal foot bone stick out and causing the big toe to point towards the other toes. Thick, hardened skin or calluses often form on the second toe and underneath the big toe. A bunion can also make it difficult to find comfortable shoes, as they change the structure of the feet. They can also cause pain and discomfort while walking or standing. Bunions tend to get worse without treatment, so if you have bunions, it is suggested that you seek the care of a podiatrist to stop or slow their progression and get the right treatment for you.
If you are suffering from bunion pain, contact Glenn Davison, DPM of Advanced Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
Symptoms
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions are large bony bumps at the base of the big toe. Medically known as hallux valgus, a bunion is a misalignment of the metatarsophalangeal joint, or big toe joint. The misalignment will generally worsen with time if left untreated.
The exact cause of bunions is unknown, with genetics seen as a potential cause. High heels and poorly-fitted footwear, rheumatoid arthritis, and heredity all seem to be potential factors behind the exacerbation of bunions. Women have been found to be more likely to develop bunions in comparison to men.
Bunions do not always produce symptoms. The best way to tell is if the big toe is pushing up against the next toe and there is a large protrusion at the base of the big toe. You may or may not feel pain. Redness, swelling, and restricted movement of the big toe may be present as well.
Podiatrists use a variety of methods to diagnose bunions. If there are symptoms present, podiatrists will first consider that it is a bunion. If not, a physical examination will be conducted to check function of the big toe. Finally, an X-ray may be taken to view the extent of the bunion and confirm it is a bunion.
Typically, nonsurgical methods are used to treat bunions, unless the bunion has become too misaligned. Orthotics, icing and resting the foot, roomier and better fitted shoes, taping the foot, and pain medication are usually utilized first. If the bunion doesn’t go away or causes extreme pain, surgery may be required. Surgeons will either remove part of the swollen tissue or bone to straighten the toe out.
If you have a bunion, it is recommended to see a podiatrist. The longer it is left untreated, the worse it may get. Podiatrists can properly diagnose and treat a bunion before it gets worse.
Tarsal tunnel syndrome is a condition in which there is a compression of the posterior tibial nerve. The posterior tibial nerve runs along the inside of the ankle into the foot. Tarsal tunnel syndrome is named for the tarsal tunnel, which is a thin space along the inside of the ankle beside the ankle bones. This space contains various nerves, arteries, and tendons, and includes the posterior tibial nerve. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome the tibial nerve is compressed, causing tingling or burning, numbness, and pain.
Common causes of tarsal tunnel syndrome involve pressure or an injury. Injuries that produce inflammation and swelling in or around the tunnel may place pressure on the posterior tibial nerve. Direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or trauma to the tibial nerve, can result in tarsal tunnel syndrome. Diseases that damage nerves, such as diabetes or arthritis, may cause tarsal tunnel syndrome. Those with flat feet are at risk for developing the condition, as the extra pressure and strain placed on the foot may compress the posterior tibial nerve.
Feeling different sensations in the foot at different times is a common symptom of tarsal tunnel syndrome. An afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg. Symptoms are primarily felt on bottom of the foot and/or the inside of the ankle. Symptoms can appear suddenly and may occur due to overuse of the foot.
To diagnose tarsal tunnel syndrome, your podiatrist may examine the foot and tap the posterior tibial nerve to see if symptoms surface. He or she may also order an MRI to determine if a mass is present.
Treating tarsal tunnel syndrome will depend on the decision of your podiatrist. Multiple options are available, however, and can include rest, ice, immobilization, oral medications such as anti-inflammatory drugs (NSAIDS), physical therapy, injection therapy, orthotics, supportive shoes, braces, and surgery.
Tarsal tunnel syndrome can occur when the posterior tibial nerve that runs along the back of the ankle is pinched due to swelling or trauma. This can lead to symptoms that may include tingling, numbness, burning, or shooting pain in the affected leg. While anybody can get tarsal tunnel syndrome, it most frequently affects adults, and particularly those who have arthritis and other systemic diseases or previous injuries to the ankle area. To diagnose this condition, a podiatrist may take your medical history, conduct a physical examination, and perform a nerve conduction study or EMG. Imaging studies, like MRIs, may be used to rule out other causes for your symptoms. If you are experiencing any lower limb pain, it is suggested that you see a podiatrist.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Glenn Davison, DPM of Advanced Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
The Effects of Tarsal Tunnel Syndrome
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
 Pain felt from sesamoiditis is generally located under the big toe on the ball of the foot. The two sesamoid bones located under the base of the big toe are similar to the size of jelly beans, and they can become inflamed if an injury should occur. Patients with sesamoiditis often describe experiencing a burning pain. Sesamoiditis may have a particularly negative effect on people who enjoy running. It may feel similar to having a pebble in your shoe, and the area can appear to be swollen. Mild relief may be found when the toes and tendons are stretched several times per day. To help figure out the best treatment plan for you and to gain helpful preventative tips, please consult with a podiatrist.
Pain felt from sesamoiditis is generally located under the big toe on the ball of the foot. The two sesamoid bones located under the base of the big toe are similar to the size of jelly beans, and they can become inflamed if an injury should occur. Patients with sesamoiditis often describe experiencing a burning pain. Sesamoiditis may have a particularly negative effect on people who enjoy running. It may feel similar to having a pebble in your shoe, and the area can appear to be swollen. Mild relief may be found when the toes and tendons are stretched several times per day. To help figure out the best treatment plan for you and to gain helpful preventative tips, please consult with a podiatrist.
Sesamoiditis is an unpleasant foot condition characterized by pain in the balls of the feet. If you think you’re struggling with sesamoiditis, contact Glenn Davison, DPM of Advanced Podiatry. Our doctor will treat your condition thoroughly and effectively.
Sesamoiditis
Sesamoiditis is a condition of the foot that affects the ball of the foot. It is more common in younger people than it is in older people. It can also occur with people who have begun a new exercise program, since their bodies are adjusting to the new physical regimen. Pain may also be caused by the inflammation of tendons surrounding the bones. It is important to seek treatment in its early stages because if you ignore the pain, this condition can lead to more serious problems such as severe irritation and bone fractures.
Causes of Sesamoiditis
Treatment for sesamoiditis is non-invasive and simple. Doctors may recommend a strict rest period where the patient forgoes most physical activity. This will help give the patient time to heal their feet through limited activity. For serious cases, it is best to speak with your doctor to determine a treatment option that will help your specific needs.
If you have any questions please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Sesamoiditis is a condition in which the sesamoid bones in the forefoot become inflamed from physical activity. Sesamoid bones are bones that are not connected to other bones but are located in tendons or muscle. Two of these sesamoid bones are very small and located on the underside of the foot near the big toe. Athletes such as runners, baseball and football players, and dancers are likely to experience sesamoiditis. Those with high arched feet, flat feet, or runners who run on the ball of their foot are also prone to suffer from sesamoiditis.
Symptoms include pain or throbbing on the ball of the foot near the big toe. The pain generally starts with a mild throbbing but gradually builds up to shooting pain. Bruising, swelling, and redness are possible, but in most cases, these symptoms are not present. However, moving the big toe can result in pain and difficulty.
To conduct a diagnosis, the podiatrist will examine the ball of the foot and big toe. They will look for any outliers and check the movement of the toe. X-rays will be taken to rule out any other conditions and ensure that it is sesamoiditis.
Treatment for sesamoiditis is generally mild and includes rest, anti-inflammatory and pain medication, and ice treatments to deal with the swelling and pain. Orthotics may be needed with people who have flat or high arched feet to relieve pressure off the bones. In some cases the toe will be taped and immobilized to allow healing. The podiatrist may also decide to use a steroid injection to help with swelling as well. If you have sesamoiditis, you shouldn’t engage in any intensive activity, as it may inflame the area and worsen your pain. If the sesamoid bone has fractured, surgery may be required to remove the sesamoid bone.
If you are suffering from sesamoiditis or are experiencing symptoms similar to sesamoiditis, you should stop all physical activity that puts strain on the area. Furthermore you should see a podiatrist for a diagnosis to see if you have sesamoiditis.
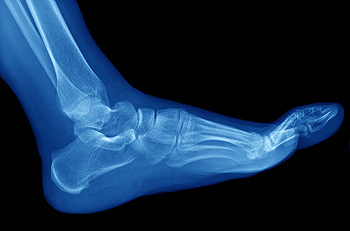 There are 26 bones in the foot and recognizing the symptoms of a broken bone is important for ensuring the overall health of your feet. A broken foot can be as simple as a small hairline fracture (such as a stress fracture), or it can be a severe break that tears or pierces the skin. The most common symptoms of a broken foot are pain, swelling, and bruising. Other common signs include a snapping or grinding sensation at the time of injury, difficulty or pain when moving the affected foot, inability to bear weight on the foot, tenderness from touching the injury, and difficulty walking. Telling the difference between a broken foot and a sprained foot can be difficult. That is why anyone who believes that they may have a broken foot should consult with a podiatrist for a proper diagnosis. A podiatrist will also be able to help provide the best treatment options for the broken bone.
There are 26 bones in the foot and recognizing the symptoms of a broken bone is important for ensuring the overall health of your feet. A broken foot can be as simple as a small hairline fracture (such as a stress fracture), or it can be a severe break that tears or pierces the skin. The most common symptoms of a broken foot are pain, swelling, and bruising. Other common signs include a snapping or grinding sensation at the time of injury, difficulty or pain when moving the affected foot, inability to bear weight on the foot, tenderness from touching the injury, and difficulty walking. Telling the difference between a broken foot and a sprained foot can be difficult. That is why anyone who believes that they may have a broken foot should consult with a podiatrist for a proper diagnosis. A podiatrist will also be able to help provide the best treatment options for the broken bone.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact Glenn Davison, DPM from Advanced Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The human foot has 26 different bones, and the foot is divided into three parts: the hindfoot, the midfoot, and the forefoot. Each section of the foot is composed of a different amount of bones. For instance, the forefoot is made up of 19 bones. The midfoot is composed of five smaller bones called the navicular, cuboid, and three cuneiform bones. Lastly, the hindfoot is made up of only the talus and the calcaneus. The feet tend to be vulnerable to slipping and twisting; consequently, fractured bones within the foot are common. When a bone gets crushed, bent, twisted, or stretched it may become broken.
Many foot fractures occur through an accident or trauma. More specifically, common causes for broken feet are car accidents, falls, missteps, or overuse. If you have a broken ankle or foot, you may have one or more of the following symptoms: throbbing pain, swelling, bruising, tenderness, deformities, and difficulty walking.
There are some factors that may put you at a higher risk of developing a broken foot. People who participate in high-impact sports are more likely to develop foot fractures because of the stresses, direct blows, and twisting injuries involved in gameplay. Additionally, those who suddenly increase their activity level are more likely to suffer a stress fracture.
Unfortunately, there are different complications that may arise because of a foot fracture. For instance, arthritis may be caused by fractures that extend into the joints. Bone infections are also possible in open fractures due to the bone being exposed to bacteria. However, there are ways you can help prevent yourself from breaking your foot. One way to avoid fractures is to wear proper footwear. If you plan on going on a run, you should wear running shoes. You should also replace your shoes if you notice that they are becoming worn out. For runners, it is best to replace shoes every 300 to 400 miles.
Treatment for foot fractures usually consists of rest, ice, elevation, and compression (RICE). If you plan on wrapping your foot, try not to wrap it too tightly because doing so may cut off blood supply in the foot. You should also avoid walking on the fractured foot.
If you suspect you have a broken foot, you should see your podiatrist right away. It is important that you have someone bring you to your doctor, since driving with a broken foot can be dangerous. You should especially seek urgent care if you are experiencing numbness, pain, or deformities in your foot.
Flip flops may be an easy, breezy accessory for warm weather, but there are many reasons why they are not good for your feet. They offer little to no support or cushioning which can lead to heel pain and problems with your Achilles tendons. You are more likely to trip wearing flip flops, and they can lead to tired, achy feet. They offer no protection from injuries or sun exposure. The worst part is that they can change your foot biomechanics and posture. Your toe muscles need to continuously grip them to keep them on, and they shorten your gait and turn your ankles inward. Contact a podiatrist if you have any pain, instability, or other problems in your feet or ankles caused by flip flops.
Flip-flops are not always the best choice of footwear. If you have any concerns about your feet or ankles, contact Glenn Davison, DPM from Advanced Podiatry. Our doctor will assist you with all of your foot and ankle needs.
Flip-Flops and Feet
When the weather starts warming up, people enjoy wearing flip-flops. Flip-flops are comfortable, stylish, and easy to slip on and off; they're perfect for any summer beach goer. However, these shoes can cause harm to the feet.
How Can Flip-Flops Affect Me Long-Term?
Are There Injuries Associated with Flip-Flops?
Yes. Since flip-flops are relatively weak and do not provide the same amount of support as sneakers, people who wear flip-flops regularly are more susceptible to injuries. On top of that, the open nature of the shoe makes your feet more prone to other problems, such as cuts and even infections. Common injuries and ailments include:
I like Wearing Flip-Flops. Are There Safe Alternatives?
When buying flip-flops, try to find ones that have sturdy soles and that are made of high-quality materials that will support for your feet. These flip-flops will cost more but will also last longer as a result.
If you have any questions please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.