NJ (908) 688-5577
NY (212) 737-2528
Athlete’s foot, or tinea pedis, is a skin disease caused by a fungal infection. The infection typically occurs between the toes, and the feet are most subject to this disease because shoes best create the warm, dark, and moist environment in which fungus thrives. Other areas that create a similar environment, such as swimming pools, public showers, and locker rooms; can also promote fungi growth.
Symptoms of athlete’s foot include dry skin, itching, scaling, inflammation, and blistering. Sometimes, blisters can evolve into the cracks or breaks in the skin. The exposed tissue can then create pain, swelling, and discharge. The spread of infection can cause itching and burning as well.
While athlete’s foot commonly occurs between the toes, it may also spread to the toenails or soles of the feet. Other parts of the body, such as the groin or underarms, can also become infected if they are touched after the original area of infection is scratched. Aside from physical contact, athlete’s foot can also spread through the contamination of footwear, clothing or bedsheets.
Proper foot hygiene is essential in preventing athlete’s foot. You can prevent the fungus from spreading by frequently washing your feet using soap and water, thoroughly drying the feet between the toes, changing shoes and socks every day to reduce moisture, and ensuring that bathroom and shower floors are disinfected. Other tips include using shower shoes, avoiding walking barefoot in public environments, wearing light and airy shoes, and wearing socks that keep the feet dry.
While treatment for athlete’s foot can involve topical or oral antifungal drugs, mild cases of the infection can be treated by dusting foot powder in shoes and socks. Any treatment used can be supplemented by frequently bathing the feet and drying the toes. If proper foot hygiene and self-care do not ease your case of athlete’s foot, contact your podiatrist. He will determine if the underlying cause of your condition is truly a fungus. If that is the case, a comprehensive treatment plan may be suggested with the inclusion of prescription antifungal medications.
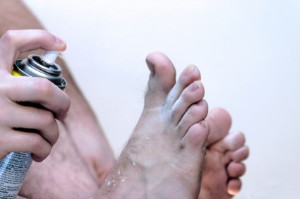 If you notice a rash on the skin of your feet, mainly between the toes, that is red, itchy, scaly or dry, it may be a sign of a fungal infection known as athlete’s foot. Athlete’s foot can cause other symptoms such as a foul odor, cracked and peeling skin, and a burning sensation. The fungi that cause athlete’s foot often thrive in warm and moist environments which means that it often spreads in areas such as communal showers or public pools. Other ways athlete’s foot can spread include sharing items that touch the feet, as well as touching the infected area directly. Patients who believe that they may have athlete’s foot should consult with a podiatrist for treatment in order to clear the infection and prevent it from spreading.
If you notice a rash on the skin of your feet, mainly between the toes, that is red, itchy, scaly or dry, it may be a sign of a fungal infection known as athlete’s foot. Athlete’s foot can cause other symptoms such as a foul odor, cracked and peeling skin, and a burning sensation. The fungi that cause athlete’s foot often thrive in warm and moist environments which means that it often spreads in areas such as communal showers or public pools. Other ways athlete’s foot can spread include sharing items that touch the feet, as well as touching the infected area directly. Patients who believe that they may have athlete’s foot should consult with a podiatrist for treatment in order to clear the infection and prevent it from spreading.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with Glenn Davison, DPM from Advanced Podiatry. Our doctor will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Gout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint.
The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
This form of arthritis, being particularly painful, is the leftover uric acid crystallizing in the blood stream. The crystallized uric acid then travels to the space between joints where they rub, causing friction when the patient moves. Symptoms include: pain, redness, swelling, and inflammation. Additional side effects may include fatigue and fever, although reports of these effects are very rare. Some patients have reported that pain may intensify when the temperature drops, such as when you sleep.
Most cases of gout are easily diagnosed by a podiatrist’s assessment of the various symptoms. Defined tests can also be performed. A blood test to detect elevated levels of uric acid is often used as well as an x-ray to diagnose visible and chronic gout.
Treatment for gout simply means eliminating symptoms. Non-steroid anti-inflammatory drugs or NSAIDs (Colchicine and other corticosteroid drugs, etc.) will quell the redness, the swelling, and the inflammation. However, managing your diet, lifestyle changes, and using preventative drugs are all helpful toward fully combating the most severe cases.
Those that lead an inactive lifestyle are at a higher risk for gout. Any amount of exercise decreases the probability of repeat encounters with the condition. Reducing your consumption of red meat, sea food, and fructose-sweetened drinks also reduces the likelihood of chronic gout as well.
Ingesting Vitamin C, coffee, and particular dairy products can help with maintaining a healthy lifestyle. There are new drugs out on the market that inhibit the body’s production of uric acid-producing enzymes. However, reducing or eliminating your overall levels of uric acid is the best remedy to ensuring you lead a gout-free life.
If you suffer from sudden pain, swelling, tenderness, heat, and stiffness in the joint of your big toe, you may have gout. This condition is an inflammatory form of arthritis where excess uric acid forms hardened crystals in the joints. The big toe is usually where gout occurs. People most at risk of developing gout are those with diabetes, hypertension, obesity, kidney dysfunction, or a genetic predisposition to it. Some believe that eating foods that are rich in purines can also contribute to gout’s formation in a person’s body. Uric acid is a byproduct of the body’s process of breaking down purines. People who suspect they have gout should consult with a podiatrist who can not only diagnose the condition, but help manage pain with anti-inflammatory medicine, make dietary recommendations, and even remove uric crystals in severe cases.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Glenn Davison, DPM from Advanced Podiatry. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
Risk Factors
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ankle sprains occur when ligaments that support the ankle stretch beyond their limits and tear. These types of injuries are very common and can occur in people of all ages. Sprains may range from mild to severe, depending on how much damage is done to the ligaments. If a sprain goes untreated, a more severe sprain may occur which can further damage the ankle. Repeated ankle sprains can lead to chronic ankle pain.
There are some risk factors that can increase your risk of suffering a sprained ankle. Those who participate in sports, walk on uneven surfaces, have a prior ankle injury, are in poor physical condition, or wear improper shoes are more likely to get a sprained ankle.
There are a few symptoms to look out for if you suspect you are suffering from a sprained ankle. Some common symptoms are swelling, bruising, tenderness, and instability of the ankle. In cases where the tearing of the ligaments is severe, there may be a “popping” sound when the strain occurs.
The RICE method is proven to be effective in treating ankle sprains. RICE stands for Rest, Ice, Compression, and Elevation. Rest is important for treatment, especially within the first 24 to 48 hours. You should also ice your sprained ankle for the first 48 hours for 20 minutes at a time. A small piece of cloth should be placed between the ice and the affected area. For the compression step, you should wear a brace that is snug, but not too tight that it cuts off circulation. When choosing a brace, be sure to choose one that is suitable for the type of ankle sprain you have. Lastly, you should elevate your foot above the heart as often as possible.
After you treat a sprain, you should go through rehabilitation to prevent the injury from occurring again. There are three phases to the rehab process. The first phase involves resting, protecting, and reducing the swelling of the injury. The second phase consists of restoring the ankle’s flexibility, range of motion, and strength. The third phase consists of slowly returning to activity and maintenance exercises.
If you suspect you have an ankle sprain, you shouldn’t hesitate to consult with your podiatrist. Your podiatrist will be able to give you a proper diagnosis and a suitable treatment option for your condition.
Though it often affects athletes, an ankle sprain can happen to anyone, anytime, and anywhere. Sometimes all it takes to sprain an ankle is to land awkwardly after a jump, or twist your ankle too much as you step off a curb. Symptoms of an ankle sprain include pain in the ankle, particularly when trying to move it or put weight on it, and swelling. If you are feeling these symptoms following an injury, stop what you are doing and rest the affected ankle. Use ice packs wrapped in a towel and elevate your injured ankle to reduce swelling. You can also compress the ankle by wrapping it with an elastic bandage. A sprained ankle needs to heal fully and properly to avoid re-injury. If you have sprained your ankle, it is strongly suggested that you seek the care of a podiatrist.
Ankle sprains are common but need immediate attention. If you need your feet checked, contact Glenn Davison, DPM from Advanced Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains take place when the ligaments in your ankle are torn or stretched beyond their limits. There are multiple ways that the ankle can become injured, including twisting or rolling over onto your ankle, putting undue stress on it, or causing trauma to the ankle itself.
What Are the Symptoms?
Preventing a Sprain
Treatment of a Sprain
Treatment of a sprain depends on the severity. Many times, people are told to rest and remain off their feet completely, while others are given an air cast. If the sprain is very severe, surgery may be required.
If you have suffered an ankle sprain previously, you may want to consider additional support such as a brace and regular exercises to strengthen the ankle.
If you have any questions please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar fasciitis, the inflammation of the ligament that runs along the bottom of the foot and connects the toes to the heel bone, is a common cause of heel pain. When the plantar fascia is injured through repetitive strain, excessive exercise, prolonged standing, wearing uncomfortable shoes, or obesity, it may lead to stabbing heel pain that is typically at its worst when taking the first few steps after a long rest. Other possible causes of plantar fasciitis include structural abnormalities in the foot, such as having flat feet, high arches, overpronation, or leg length differences. Foot changes associated with aging or pregnancy may also be to blame in some cases. If you are suffering from heel pain, don’t hesitate to schedule an appointment with a podiatrist near you.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Glenn Davison, DPM from Advanced Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
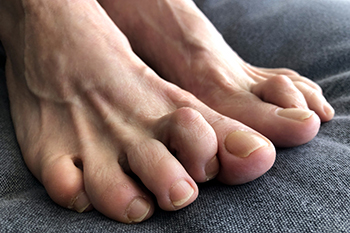 When the toes are forced to curl downwards due to the middle joints of the toes tightening up, they form what is known as a hammertoe. Hammertoes, which can affect any toe but the big toe, are often most uncomfortable at the top of the toes where they rub against shoes. There are two types of hammertoes and they are both affected by the toe’s mobility. Flexible hammertoes can be manually straightened out, but rigid hammertoes can not be straightened out and they are very painful and limited in movement. Patients who are struggling with a hammertoe should make sure their shoes have a high and wide toe box to give the toes enough space. Persistent hammertoes should be checked by a podiatrist for possible treatment options that may include surgery.
When the toes are forced to curl downwards due to the middle joints of the toes tightening up, they form what is known as a hammertoe. Hammertoes, which can affect any toe but the big toe, are often most uncomfortable at the top of the toes where they rub against shoes. There are two types of hammertoes and they are both affected by the toe’s mobility. Flexible hammertoes can be manually straightened out, but rigid hammertoes can not be straightened out and they are very painful and limited in movement. Patients who are struggling with a hammertoe should make sure their shoes have a high and wide toe box to give the toes enough space. Persistent hammertoes should be checked by a podiatrist for possible treatment options that may include surgery.
Hammertoes can be a painful condition to live with. For more information, contact Glenn Davison, DPM of Advanced Podiatry. Our doctor will answer any of your foot- and ankle-related questions.
Hammertoe
Hammertoe is a foot deformity that occurs due to an imbalance in the muscles, tendons, or ligaments that normally hold the toe straight. It can be caused by the type of shoes you wear, your foot structure, trauma, and certain disease processes.
Symptoms
Risk Factors
Treatment
If you have hammertoe, you should change into a more comfortable shoe that provides enough room for your toes. Exercises such as picking up marbles may strengthen and stretch your toe muscles. Nevertheless, it is important to seek assistance from a podiatrist in order to determine the severity of your hammertoe and see which treatment option will work best for you.
If you have any questions, please feel free to contact our offices located in Union, NJ and New York . We offer the newest diagnostic and treatment technologies for all your foot care needs.